Understanding Psoriatic Arthritis: Causes, Symptoms, and Treatment
Psoriatic arthritis. It’s a condition that affects millions of people worldwide, yet many still don’t fully understand what it is or how it can impact their lives. If you or someone you know has been diagnosed with psoriatic arthritis, this blog post is for you. We’re diving deep into the causes, symptoms, and treatment options available to help you better manage this chronic inflammatory disease.
But before we get started, let’s debunk a common misconception – psoriatic arthritis isn’t just another type of arthritis. It’s actually a unique combination of joint inflammation and skin problems that often accompanies the skin condition known as psoriasis. So if you’ve been dealing with those pesky plaques on your skin along with painful joints, keep reading because we’ve got all the information you need to navigate through this complex condition.
From understanding the different types of psoriasis associated with psoriatic arthritis to exploring various treatment approaches and lifestyle management tips, we’ll cover everything in detail so that by the end of this article, you’ll have a clearer picture of what lies ahead on your journey towards relief and improved quality of life. So let’s jump right in and unravel the mysteries surrounding psoriatic arthritis!
Overview
Psoriatic arthritis is a condition that combines joint inflammation with the skin disorder psoriasis. Unlike other forms of arthritis, it’s not solely focused on the joints. Psoriatic arthritis can affect various parts of the body, including the fingers, toes, spine, and even the eyes.
People living with this condition may experience symptoms such as joint pain, stiffness, swelling, and fatigue. The severity of these symptoms can vary from person to person and may come and go in flare-ups. Understanding how psoriatic arthritis affects your body is crucial for effective management and finding relief from its impact on daily life.
Symptoms
Psoriatic arthritis can cause a range of symptoms that vary from person to person. Common symptoms include joint pain, stiffness, and swelling. These symptoms often affect the fingers, toes, wrists, knees, or ankles. Some individuals may also experience fatigue and tenderness in the affected joints.
In addition to joint problems, psoriatic arthritis can also lead to skin issues such as redness and inflammation around the joints. Other symptoms may include nail changes like pitting or separation from the nail bed. It’s important to note that these symptoms can come and go over time or worsen during flare-ups. If you’re experiencing any of these signs, it’s crucial to seek medical advice for proper diagnosis and treatment options tailored specifically to your condition.
Causes
Psoriatic arthritis is an inflammatory condition that affects both the skin and joints. While the exact cause is still unknown, researchers believe it involves a combination of genetic and environmental factors.
Genetics play a role in psoriatic arthritis, as individuals with a family history of the disease are more likely to develop it themselves. Environmental triggers such as infections or injuries can also contribute to its onset. Additionally, an overactive immune system plays a key role in the development of psoriatic arthritis, causing inflammation throughout the body.
Understanding the causes of psoriatic arthritis can help healthcare professionals better diagnose and treat this chronic condition. By identifying potential risk factors and triggers, individuals at risk may be able to take proactive steps to manage their symptoms and improve their overall quality of life.
Diagnosis
Diagnosis of psoriatic arthritis can be challenging as it shares symptoms with other types of arthritis. Your doctor will consider your medical history, perform a physical examination, and order tests to confirm the diagnosis. During the physical exam, they may look for signs of joint swelling, tenderness, or skin lesions. They may also assess your range of motion and ask about any associated symptoms you’re experiencing. To confirm the diagnosis, blood tests may be done to check for markers such as rheumatoid factor or antibodies related to psoriasis. Imaging tests like X-rays or MRI scans might also be used to evaluate joint damage and inflammation.
Receiving an accurate diagnosis is crucial in managing psoriatic arthritis effectively. It allows healthcare professionals to tailor treatment plans based on individual needs and reduce potential complications associated with untreated or misdiagnosed conditions
Plaque Psoriasis
Plaque psoriasis is the most common form of psoriasis, affecting millions of people worldwide. It is characterized by raised, red patches covered with a silvery white buildup of dead skin cells, known as plaques. These plaques can appear anywhere on the body but are commonly found on the scalp, elbows, knees, and lower back.
Living with plaque psoriasis can be challenging both physically and emotionally. The constant itching and discomfort can make everyday tasks difficult to bear. Moreover, the visible nature of the condition may lead to self-consciousness and low self-esteem in those affected. However, with proper management and treatment options available today, individuals with plaque psoriasis can find relief from symptoms and improve their quality of life.
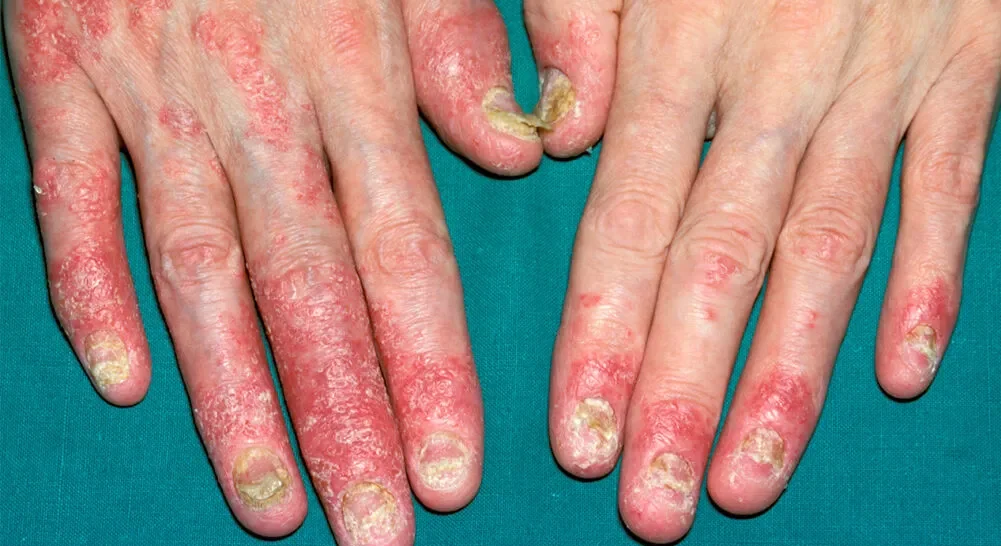
Psoriasis on the Nails
Psoriasis on the Nails is a common manifestation of psoriatic arthritis. It occurs when the skin condition affects the nails, causing changes in their appearance and texture.
One of the most noticeable signs is pitting, which appears as small depressions or dents on the surface of the nails. Additionally, patients may experience discoloration, with patches of yellowish-brown or white appearing on the nail bed. The nails can also become thickened and crumbly, making them more prone to breakage.
Psoriasis on the Nails can be uncomfortable and may affect daily activities such as grasping objects or performing hygiene tasks. If you notice any changes in your nails that resemble these symptoms, it’s essential to consult a healthcare professional for an accurate diagnosis and appropriate treatment options.
Associated Symptoms
Psoriatic arthritis is more than just joint pain. It often comes with a range of associated symptoms that can affect various parts of the body. These symptoms can vary from person to person, but some common ones include fatigue, swollen fingers or toes, stiffness in the joints (especially in the morning), and even eye inflammation.
In addition to these physical symptoms, psoriatic arthritis can also have an impact on mental health. Many people with this condition experience depression and anxiety due to the chronic pain and discomfort they endure on a daily basis. It’s important to address both the physical and emotional aspects of psoriatic arthritis when seeking treatment and support.
Non-Urgent Advice: See a GP if
If you’re experiencing symptoms that could potentially be related to psoriatic arthritis, it’s important to seek medical advice. While not urgent, it is still recommended to see a general practitioner (GP) if you notice persistent joint pain or swelling, especially if it affects multiple joints. Additionally, if you have been diagnosed with psoriasis and are now developing new symptoms such as stiffness in the morning or difficulty moving your joints, it’s essential to get checked out by a healthcare professional.
A GP can assess your symptoms and refer you to a specialist for further evaluation and diagnosis. Remember, early detection and treatment play a crucial role in managing psoriatic arthritis effectively. So don’t hesitate to reach out for non-urgent medical advice when needed!
Check if You Have Psoriatic Arthritis
Psoriatic arthritis can often be mistaken for other types of arthritis or even just joint pain. So, how do you know if your symptoms are indicative of psoriatic arthritis? Here are a few signs to look out for.
First and foremost, if you have been diagnosed with psoriasis – a chronic skin condition characterized by red, scaly patches – and you’re experiencing joint pain, it could be an indication of psoriatic arthritis. Additionally, swelling in the fingers or toes (known as dactylitis), stiffness in the morning that lasts more than 30 minutes, or pain in areas where tendons and ligaments attach to bones (such as the Achilles tendon) may also point towards this condition. If any of these symptoms resonate with you, it’s important to seek medical advice from your healthcare provider for further evaluation and diagnosis.
What Happens at Your Appointment
When you have an appointment to discuss your psoriatic arthritis, it’s important to know what to expect. The first thing that will happen is a discussion about your symptoms and medical history. Your healthcare provider will ask detailed questions about the type of pain you’re experiencing, any joint stiffness or swelling, and how these symptoms are affecting your daily life.
Afterwards, they will likely perform a physical examination, focusing on the affected joints and checking for signs of inflammation or damage. They may also order blood tests to look for markers of inflammation or other conditions that could be contributing to your symptoms. Additionally, imaging tests such as x-rays or ultrasounds may be recommended to get a clearer picture of the affected joints. By gathering this information, your healthcare provider can make an accurate diagnosis and develop a personalized treatment plan tailored specifically for you!
Medicines for Psoriatic Arthritis
When it comes to treating psoriatic arthritis, medications play a crucial role in managing the symptoms and slowing down the progression of the disease. There are several types of medicines that can be prescribed by your healthcare provider, depending on the severity of your condition.
One common approach is nonsteroidal anti-inflammatory drugs (NSAIDs), which help reduce inflammation and alleviate pain. Another option is disease-modifying antirheumatic drugs (DMARDs) that work to suppress the immune system and prevent joint damage. In more severe cases, biologic response modifiers may be recommended, as these medications specifically target certain proteins involved in inflammation. It’s important to work closely with your doctor to find the right medication or combination of medications that best suit your needs.
Other Treatments for Psoriatic Arthritis
When it comes to treating psoriatic arthritis, there are several options available beyond medication. These alternative treatments can help manage symptoms and improve overall quality of life. One approach is physical therapy, which focuses on exercises and stretches to increase mobility and reduce pain. Additionally, occupational therapy can assist in finding ways to adapt daily activities for those with joint stiffness or limited movement. Other complementary therapies like acupuncture or chiropractic care may also provide relief for some individuals.
Another aspect worth exploring is lifestyle modifications. Maintaining a healthy weight through diet and regular exercise can alleviate stress on joints affected by psoriatic arthritis. Stress management techniques such as meditation or yoga might also be beneficial in reducing inflammation flare-ups. It’s essential to discuss these treatment options with your healthcare provider to determine the best course of action tailored specifically for you.
Management and Treatment
Once diagnosed with psoriatic arthritis, it’s important to develop a comprehensive management plan that addresses both the symptoms and underlying causes. This typically involves a combination of medication, lifestyle modifications, and regular monitoring.
Medications play a crucial role in managing psoriatic arthritis. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation. Disease-modifying antirheumatic drugs (DMARDs) may be prescribed to slow down joint damage progression. In more severe cases, biologic response modifiers are used to target specific components of the immune system involved in inflammation.
Lifestyle modifications are also essential for managing symptoms. Regular exercise can improve joint flexibility and overall well-being. Maintaining a healthy weight reduces stress on joints affected by psoriatic arthritis. Physical therapy and occupational therapy techniques can also be beneficial in managing pain, improving mobility, and enhancing daily functioning.
Remember to consult with your healthcare provider regularly to monitor your condition and adjust treatment as needed. With proper management strategies in place, individuals living with psoriatic arthritis can effectively control their symptoms, minimize flare-ups, and lead fulfilling lives.
Prevention
Prevention plays a crucial role in managing psoriatic arthritis. While there is no guaranteed way to prevent this condition, adopting certain lifestyle changes can help reduce the risk and improve overall well-being.
First and foremost, maintaining a healthy weight is important as excess weight puts additional stress on joints. Regular exercise not only helps with weight management but also improves joint flexibility and strength. Additionally, avoiding smoking and limiting alcohol consumption can have positive effects on both skin and joint health. Furthermore, managing stress levels through relaxation techniques or therapy may help minimize flare-ups of psoriatic arthritis symptoms.
By making these proactive choices, individuals can potentially decrease their chances of developing psoriatic arthritis or alleviate its impact on daily life. Remember that prevention strategies are most effective when combined with regular medical check-ups for early detection and proper management of any underlying conditions related to this chronic autoimmune disease.
Living with Psoriatic Arthritis
Living with Psoriatic Arthritis can be challenging, but it is possible to lead a fulfilling life. It’s important to remember that every individual’s experience with the condition is unique, and what works for one person may not work for another.
One of the key aspects of managing psoriatic arthritis is finding a treatment plan that works best for you. This may involve a combination of medications, physical therapy, exercise, and lifestyle changes. Additionally, seeking support from friends, family, or joining support groups can provide emotional assistance during difficult times. By taking proactive steps in managing your symptoms and maintaining open communication with healthcare providers, you can strive towards achieving an improved quality of life despite living with psoriatic arthritis.
Clinical Tools and Guidelines
Psoriatic arthritis is a complex condition that requires proper diagnosis and ongoing management. Fortunately, there are numerous clinical tools and guidelines available to help healthcare professionals effectively treat patients with psoriatic arthritis.
Clinical tools such as the Psoriasis Area Severity Index (PASI) can assess the severity of skin involvement in psoriasis, while the Assessment of SpondyloArthritis International Society (ASAS) criteria can aid in diagnosing axial involvement in psoriatic arthritis. These tools, along with others like joint counts and imaging studies, enable healthcare providers to accurately evaluate disease activity and progression.
Guidelines issued by organizations like the American College of Rheumatology (ACR), National Institute for Health and Care Excellence (NICE), or European League Against Rheumatism (EULAR) provide evidence-based recommendations on treatment options for psoriatic arthritis. These guidelines consider factors such as disease severity, comorbidities, patient preferences, and response to previous therapies.
Treatment approaches for psoriatic arthritis may include nonsteroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), biologic medications targeting specific immune pathways involved in inflammation, physical therapy exercises to improve range of motion and strengthen muscles around affected joints. Lifestyle modifications such as maintaining a healthy weight, regular exercise routine tailored to individual capabilities can also play an important role in managing symptoms.
Regular follow-up appointments with rheumatologists or dermatologists are crucial to monitor disease activity and adjust treatment plans accordingly. Ongoing communication between patients and their healthcare team ensures that any changes or concerns are addressed promptly.